20 May, 2009. Exactly one month since Operation #1, the bilateral lumpectomy.
Consent for the bilateral mastectomy signed, operation booked and they were about to come off.
My boobs had been the centre of my world for several months now and the morning of the ‘big operation’ was no different. There wasn’t a lot of talking though, just a very uneasy silence. I wasn’t sad, worried, upset – just anxious. My final shower with my boobs was quite surreal.
Dr D was planning to take a couple of lymph nodes just to check the cancer hadn’t become invasive. Without going into too much detail – the process of preparation for a Sentinel Node Biopsy was one of the most unpleasant experiences I’ve ever endured. Four syringes of dye injected around and into the nipple. Yes, I swore.
After hours of waiting for the dye to reach the lymph nodes I had some x-rays done. Then another long wait for the surgery to begin.
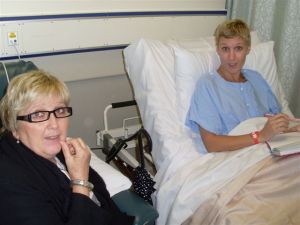
A volunteer from Cancer Council Queensland came to visit – bringing with her a heap of information for sufferers and those close to them. She also gave me a pink satin cushion – shaped like one of those neck pillows for travel, assuring me I’d find it very useful for under my arm when I woke up. I had visits from a couple of nurses I knew personally – Kay a family friend from way back, and Wendy who’s married to the boss of Channel Ten here on the Coast. In a sign of how frequently I’d been in recently, I was also on a first-name basis with the admissions nurse Dot!
I was off to theatre mid-afternoon. More familiar faces with a couple of the anaesthetic nurses from my previous surgeries.
Dr D came for that ‘last minute chat’, only this time he had a camera in hand, along with a big purple texta. As he took photos of my boobs I smiled “no need to pose Kate, I’m not getting your face” he laughed. Then with that purple pen he marked out where my boobs sat. Another one of those very strange life experiences.
I was starting to get a little groggy as I climbed from the trolley onto the table, but pulled the gown down for ‘one last look’, much to the amusement of all the medical professionals who now had my life (and boobs!), in their hands.


